 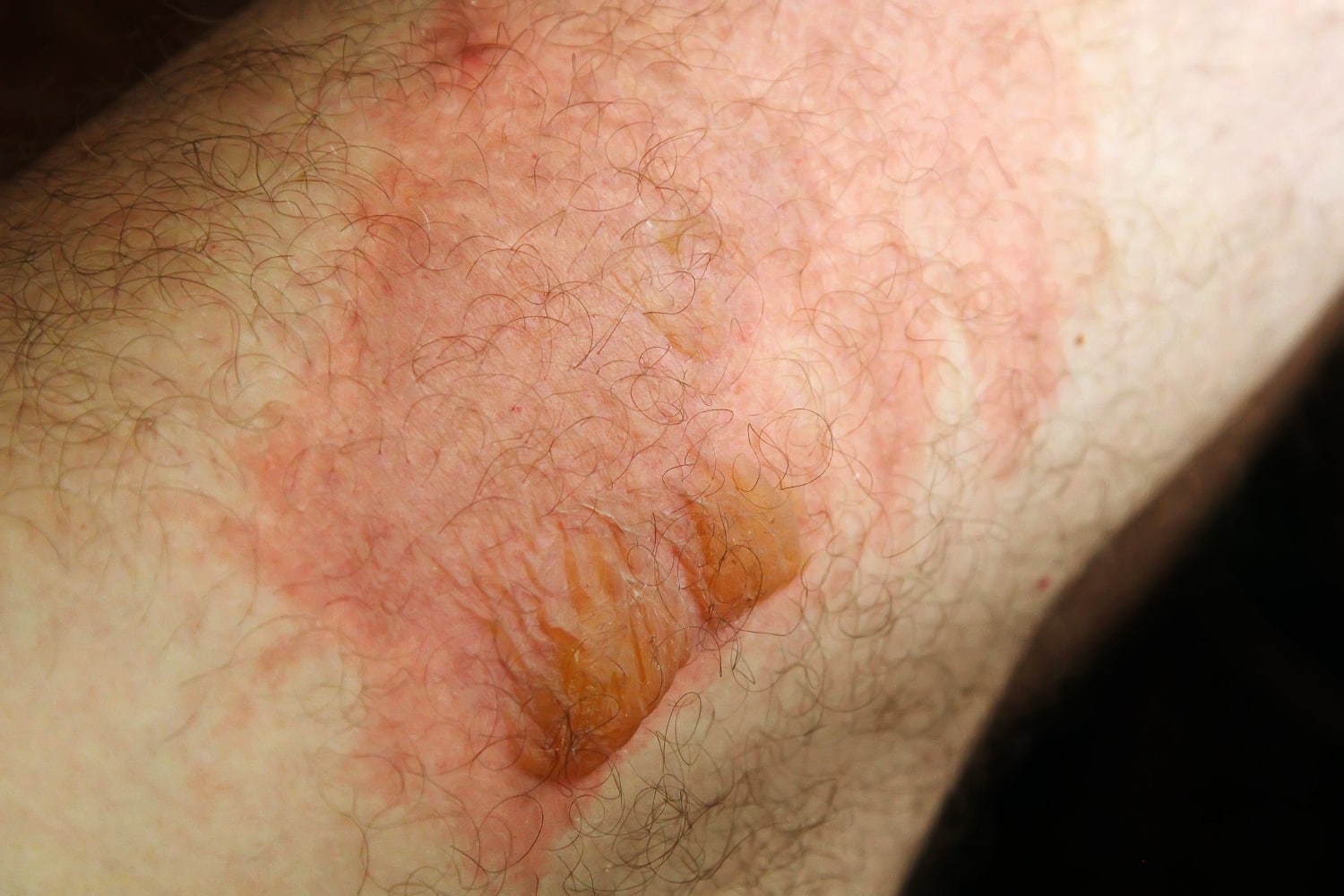
When the burn size exceeds about 25% of the body surface, interstitial edema develops in distant organs and soft tissues, mainly secondary to a combination of wound-released mediators and hypoproteinemia. The systemic response to burning is driven by the loss of the skin barrier and release of vasoactive mediators from the wound and from subsequent infection. 
A local response to burning involves not only direct tissue coagulation but also burn tissue conversion, a process where the damaged cells, rather than recover, progress to cell death, extending the depth and severity of the original injury. The activation of a pro-inflammatory cascade after a burn appears to be important in the development of subsequent immune dysfunction, bacterial translocation from the gut, susceptibility to sepsis and multiple organ failure. Severely burned skin ceases to perform its natural protective and barrier role and allows a dramatic increase in water loss and can become a portal for bacterial invasion. These are used to calculate the % of body surface area affected by burns and determine the prognosis and susceptibility to infection. This active area of research will continue to provide new topical antimicrobials for burns that will battle against growing multi-drug resistance. Various silver preparations (nanocrystalline and slow release) are the mainstay of many approaches but antimicrobial peptides, topical photodynamic therapy, chitosan preparations, new iodine delivery formulations, phage therapy and natural products such as honey and essential oils have all been tested. Animal models that are used in preclinical studies are discussed. This review will cover patented strategies that have been issued or filed with regard to new topical agents, preparations, and methods of combating burn infections. However the relentless increase in microbial resistance to antibiotics and other antimicrobials has led to a renewed search for alternative approaches to prevent and combat burn infections. 
In the 20th century the introduction of antibiotic and antifungal drugs, the use of topical antimicrobials that could be applied to burns, and widespread adoption of early excision and grafting all helped to dramatically increase survival. A number of factors such as disruption of the skin barrier, ready availability of bacterial nutrients in the burn milieu, destruction of the vascular supply to the burned skin, and systemic disturbances lead to immunosuppression combined together to make burns particularly susceptible to infection. Throughout most of history, serious burns occupying a large percentage of body surface area were an almost certain death sentence because of subsequent infection. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
